Health Care Fraud
Healthcare fraud remains one of the cornerstones of the government’s efforts to identify and prosecute claims for fraud through the use of the False Claims Act and its whistleblower provisions. Each year, billions of dollars flow through the primary government healthcare programs, Medicare and Medicaid, which reimburse providers, hospitals, pharmacies, medical device manufacturers, and others for the cost of healthcare of the elderly, the lower-income population, and those in military service.
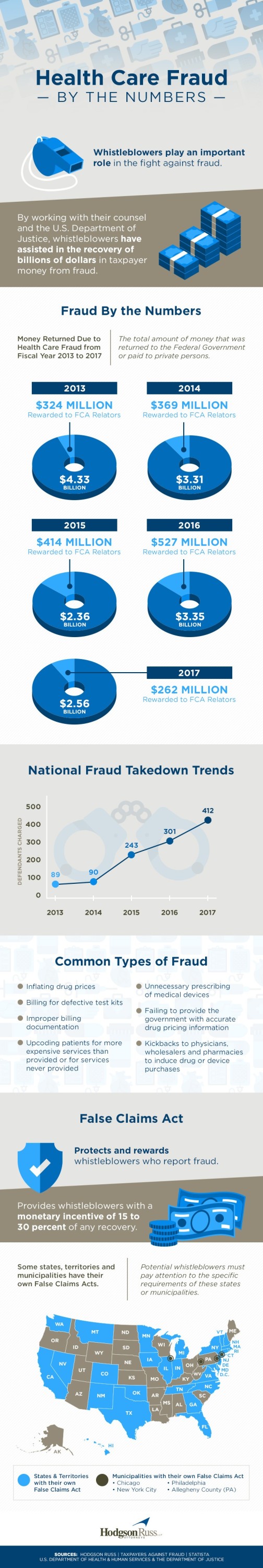
The sheer size of Medicare/Medicaid programs makes federal healthcare a target for fraud and abuse. In 2016, the government recovered $2.5 billion from the health care industry.
The scope of “healthcare fraud” under the False Claims Act is extraordinarily broad. The term includes a wide variety of substantive areas funded by Medicare/Medicaid dollars each year. By way of example, there are several areas which have seen False Claims Act enforcement actions, and even criminal charges, for fraud and abuse over the past number of years:
Areas of Medicare/Medicaid False Claims Act Enforcement
- Provider billing fraud through, for example, up-coding patients for more expensive services than actually provided, and services that were never performed;
- The billing for unnecessary services such as laboratory tests or other diagnostic treatments;
- Significant deficiencies in the quality of care in long-term care or clinical settings;
- Prescription drug fraud by both pharmaceutical companies and prescribers relating to efficacy, off-label promotion, prescription drug abuse, and provider bribery or kickbacks;
- Failing to provide accurate information to the government about drug prices;
- Unnecessary prescribing of medical devices;
- Improper billing documentation for the use of residents, interns, nurses or other assistants, and improper billing for physician training and education.
These are only a sampling of healthcare fraud and abuse cases under Federal provider programs where the False Claims Act has been used to facilitate recovery of amounts improperly paid, together with penalties and interest.
Partner with Our False Claims Act and Medicare/Medicaid Attorneys at Hodgson Russ
Hodgson Russ has vast experience both defending cases involving allegations of health care fraud under the False Claims Act and representing whistleblowers and relators exposing fraud in the Medicare and Medicare payment systems. The Firm’s unique practice has resulted in a thorough understanding of how the Medicare and Medicaid system operates, where fraud is most prevalent, and what government enforcement authorities view to be the most critical areas of concern. Hodgson Russ continues to build knowledge and experience in one of the most fertile areas for False Claims Act litigation and government scrutiny.
